The Book
Throwback Thursday Classic Post – MCCareer.org The Book – Undersea Medicine Chapter
(If you are residency trained already, you can go UMO any time. You don’t have to wait for the GME Selection Board.)
Brian M. Keuski, MD
Ian F. Eisenhauer, MD
Note: The views expressed in this chapter are those of the author(s) and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.
INTRODUCTION TO UNDERSEA MEDICAL OFFICER (UMO):
Undersea Medicine is a small community within Navy Medicine, which primarily performs special duty physicals for divers, submariners, special operators, and nuclear-trained personnel. The Undersea Medical Officer (UMO) community, and those specialized communities that utilize UMOs, are high-tempo, actively deploying units ranging from Naval Special Warfare (NSW) to submarine squadrons. The role of the UMO is a mix of the general operational medicine that is expected of all General Medical Officers tailored to the specific duty concerns germane to the communities served. UMOs receive specialized training in these two key areas to ensure that they can adequately screen service members for conditions that could jeopardize the mission or lead to harm in diving, submarine or radiation health environments.
Medical administration (medical readiness, waivers/disqualifications, and the Independent Duty Corpsman (IDC) Program) takes up the majority of your time working as a UMO. UMOs train IDCs to tackle the challenging role of independent practice in austere environments with abbreviated training. UMOs must screen service members for illness that could overwhelm an IDC’s ability, as well as prepare IDCs to take care of those illnesses that arise with minimal access to MEDEVAC or specialty care. The key to success for a UMO will hinge directly on their ability to train those Dive Medical Technicians (DMTs) and IDCs who will ultimately perform patient care in the field.
UMO STRUCTURE AND JOB OPPORTUNITIES:
The UMO Community, as noted above, is a mix of submarine and diving support, organized by TYCOM-level leadership. UMOs fill billets assigned to the Marine Corps, Submarine Squadrons, Navy Special Warfare, Navy Expeditionary Combat Command (NECC), training commands, research commands, and Military Treatment Facilities as well as shipyard clinics. Most UMO roles are clinic-based. Completion of special duty physicals and leadership/mentorship of IDCs are the primary facets of the job. Some jobs incorporate diving into their role, while others have no associated diving. The many types of UMO billets are represented by categories, below.
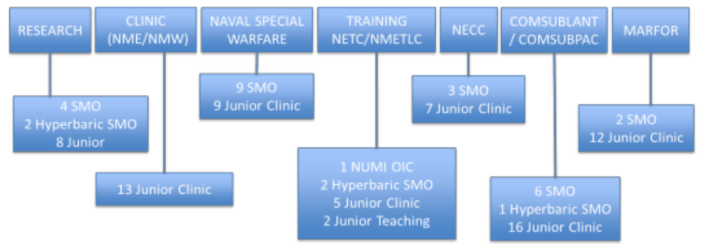
The UMO Specialty Leader (M-95, Head Undersea Medicine) is located at the Bureau of Medicine and Surgery (BUMED) in Falls Church, Virginia, and oversees all of Radiation Health and Undersea Medicine. He/she makes recommendations to the waiver authority on all waivers and disqualifications of special duty standards. While all UMOs function under the oversight of the Specialty Leader, each has an operational chain of command. They either have a senior medical officer, or directly report as special staff to line officers in their daily duties. The above outline includes billets that are designated as senior officer billets, including some who are selected from the career milestone board, such as the Naval Undersea Medical Institute Officer-in-Charge (NUMI OIC) and Naval Submarine Medical Research Laboratory Commanding Officer and Executive Officer (NSMRL CO/XO), whereas others are open to any applicant. Second tour UMOs or senior UMOs will often have more opportunity to request billets, while those billets going to first tour UMOs will be chosen by the Detailer and Specialty Leader based upon their operational status, requirements, and “needs of the Navy.”
UMO APPLICATION:
UMO applications must be completed by the end of October, and selectees will be notified in December in parallel with graduate medical education (GME) selection. In order to prepare a successful application, UMO applicants must complete: a physical examination by a UMO (MANMED 15-102, 15-106), a passing Diver Candidate Physical Screening Test (PST) (MILPERSMAN 1220-410), two letters of recommendation, and a command letter of endorsement. A complete list of requirements can be found at the NUMI Website. Notably, these requirements represent minimum standards for training, but physical fitness well in excess of the minimums should be sought for a competitive application.
https://www.med.navy.mil/sites/nmotc/numi/UMOApply/Pages/default.aspx
Prospective UMOs historically have had the most difficulty with preparation for, and successful execution of the PST with a diver, as well as a letter of recommendation from qualified UMOs. The best resources for interns are nearby fleet UMOs or prior UMOs currently in GME training at your local MTF. These individuals can help you navigate the process, offer a recommendation letter, and administer your PST. If they can’t help you, the community is often small enough that they will know others that can. If no returning UMOs are within your intern class, ask upper level residents if they know any fleet returnees. Ultimately, the website above contains the contact information for the NUMI-POC, UMOC Mailbox, and the UMO Specialty Leader, each of whom will be willing to help you locate resources if you cannot otherwise. Letters of recommendation are also often difficult to complete. UMO letters of recommendation are designed to ensure you have considered why you are applying to the program, and to offer avenues for advice as you apply. If available during your intern program, scheduling an operational rotation with a local UMO can assist with the application requirements as well as show sustained interest.
The deadline for UMO application is in October; an interested applicant should complete the application in June-August to avoid an application being disqualified for missing requirements, including issues with medical standards that take time to process.
UMO PREPARATION:
Six months is a reasonable minimum amount of time to prepare for training prior to transferring to NUMI. Preparation must include learning multiple swim strokes, gaining in-water confidence, preparing to run significant distance, as well as improving callisthenic endurance. Below are outlined some minimum goals for reaching NUMI, though some factors that lead to success in school cannot be quantified. Ultimately, confidence in the water is the most important aspect of preparation for UMO training, and this takes time.
Be prepared to pass the PST with room to spare.
The Diver PST is a minimum standard that is used to ensure that candidates are ready to train. If you do not pass this ‘test’ on day one, you will be dismissed from training. Your swim will be in a cramped pool, with a shirt and UDTs on, and without goggles.
Some suggestions for success include:
- Train without goggles.
- Train in a crowded lane where you need to navigate around other swimmers.
- Swim with shorts and a baggy T-shirt to simulate the drag from the diver uniform.
- Become proficient, if not excellent, at sidestroke.
You also need to be prepared for the other events. Note that you will do your pull-ups after having just completed swimming, sit-ups, and push-ups. This fatigue causes issues for many people. Ten consecutive pull-ups prior to NUMI is a good minimum preparation for PST to compensate for this fatigue. If you currently can’t do any pull-ups, get multiple resistance bands, attach them to a pull-up bar (buy one and put it on your door – either at work or at home), and use as many bands as are necessary to be able to complete 6-8 pullups per set. When you can do 10 in a set, drop a band (or go to a smaller one). You should do pull-ups every other day, and you should do 50-60 at a minimum, which can be consecutive or broken up. If you do this for a few months, you will gain the required strength to do the pull-ups required for the PST.
Running is an important part of preparation for the PST. Being tired from upper body workouts and the aerobic stress of the pool will set you up to be slower than usual. You should be able to run your 1.5 miles in 11 minutes or under when you are fresh. Preparation can be with daily runs of 2-3 miles with 1 run per week designed to improve speed, and 1 run designed to improve distance. Examples of speed workouts may include Tabata runs or ¼ mile sprints, with a total distance of at least 1.5-2 miles (the length of the run portion of the PST) in sprints (e.g. 8 x ¼ mile sprints at goal pace, or under 1:50 per lap for an 11 minute time).
Be prepared to run for 5 miles at about an 8 minute mile pace.
While this may seem quick, you must recognize that you will be yelling cadences, running in formation, and carrying a guide-on flag. They will run you hard. Those who are unprepared for this type of distance often suffer stress injuries (shin splints, knee pain such as patellofemoral pain syndrome, etc.), so being prepared is crucial to making it through training. While at NUMI, they may not make you run this fast, but at NDSTC, some training teams will run significantly faster and farther.
Spend time doing hypoxia training (on land).
While breath-hold training in the water without supervision is dangerous, land-based training is very helpful in preparation for UMO training. There are many apps to teach you to hold your breath; STAmina Apnea Trainer, iHoldBreath, AIDA Freediving, and others. Having some comfort with a breath-hold allows a trainee to put their focus elsewhere during training. A 1:30 second breath-hold is a great starting place prior to starting at NUMI.
Get confident in the water.
You should be able to swim a minimum of 1000 meters in a workout, with mixed in push-ups, sit-ups, and pull-ups on the side of the pool. Calisthenic exercise mixed with swimming increases aerobic stress dramatically, and should be experienced before NUMI. Familiarity with breaststroke and freestyle are also useful, despite sidestroke and breaststroke being the only authorized swim strokes for the PST. Treading water is one of the most challenging factors of aquatic adaptability, and the eggbeater kick will make treading water easier. A trainee will need to be able to tread water with hands and elbows out of the water for a minimum of one minute. While methods other than eggbeater (frog kicks, flutter kicks, etc.) may seem easier at first, these methods break down when weight is held overhead. Becoming competent and confident while treading water will serve you well in training.
NUMI/NDSTC TRAINING PIPELINE, WHAT TO EXPECT:
The Naval Undersea Medicine Institute (NUMI) in Groton, CT is home to training for prospective Undersea Medical Officers. As noted above, preparation for this nearly six month training pipeline is crucial to success in becoming a UMO. The training pipeline is broken into three phases:
PHASE 1:
The First Phase of UMO Training is built around preparation for U.S. Navy Dive training at NDSTC. While there is a lot to learn to become an effective UMO, candidate failure is most often caused by quitting (drop on request -DOR) or an inability to meet the physical standards. Phase 1 physical preparation includes daily 1.5 hour workouts at 0500 to include running, calisthenics, swimming, in-water confidence training, practicing pool ‘hits,’ and other drills. The primary goals of UMOC preparation are PST preparation and in-water confidence training. This is where you will be introduced to over-unders, a repetitive under water swimming exercise. Preparation as noted above is highly encouraged to prepare you to start these exercises. While many UMOCs want to do over-unders prior to NUMI, the risk of shallow-water blackout is significant and has led to the death of skilled individuals. It is not recommended to do in water breath hold training before the safe training environment of NUMI. It is sufficient to become a great swimmer and have a good breath-hold prior to NUMI.
The time between workouts is spent learning radiation physics and health topics to complete the Radiation Health Indoctrination (RHI) certification. This certification prepares future UMOs to care for workers in the Radiation Health Program, as it allows UMOs to complete Radiation Medical Examinations (RMEs). This exam is required for Submarine personnel and Navy Divers who perform diving operations near submarines. The RHI Program also prepares UMOs to be the first line of defense in the event of a nuclear/radiologic casualty. Similarly, special duty physicals are introduced, an exam that certifies that specialized forces – including submariners, special warfare personnel, divers, radiation workers, and others – are able to complete their job effectively and safely without risking the safety of the mission or of the other crew.
UMOCs learn submarine medicine topics in phase I. In the submarine force, no person does a single job; it is the role of the entire crew to complete their main task, as well as to be prepared to address casualties, including fighting fires, addressing flooding, and even escaping the submarine. UMOCs complete training in these areas to understand ship systems and to be prepared to assist in these scenarios when/if they are aboard. UMOCs are also introduced to submarine culture and the hazards associated with submarine life.
PHASE 2:
The Second Phase of UMO training occurs on TAD orders to the Naval Diving and Salvage Training Center at the Center for Explosive Ordnance Disposal and Diving (CEODD). Prospective UMOs train like every other Navy Diver candidate with physical training both on land and in the water. Comfort in the water under extreme conditions is attained by breath-hold diving, treading with and without weights, surface swimming, teamwork drills, and many more activities. Training is built to ensure that candidates are sufficiently comfortable and calm in the water to train with equipment that can be dangerous if a diver were to panic. It should be noted that while traditionally this is where students fail out of the course, proper mental and physical preparation will prepare the vast majority of candidates.
The training includes qualification on the diving equipment used in the U.S. Navy. Competence with each piece of equipment is tested in both classroom and pool settings, to include SCUBA, KM-37 (Hard Hat Diving), and Mk-20 (full face-mask). There are also shorter familiarizations to re-breather equipment used by our forces. Most importantly for medical personnel, the course includes the Recognition and Treatment (R&T) of diving casualties course, which teaches candidates the medical knowledge required for treating diving related injuries. Topics span from basic dive physics to the latest theories on decompression sickness (aka ‘The Bends’), oxygen toxicity, and many other illnesses that can be seen in Navy Diving.
PHASE 3:
UMO training culminates in Groton, CT where comprehensive Oral Boards are performed for each candidate. Overseen by Naval Reactors, the nuclear power leadership of the U.S. Navy, this board includes questions about radiation health examinations, IDC oversight, special duty physicals, and diving related injuries. This phase also includes leadership education, operational medicine lectures, and helpful education in basic medical division officer roles and responsibilities. Most important to UMOs during this phase is assignment to a billet. While the process is variable, ranging from selection based upon course rank (merit-based) to direct assignment by the detailer, the process ultimately requires patience, as most UMOCs are post-intern physicians and have not yet experienced the flexible nature of Navy Orders. Once verbally assigned a billet, there are often multiple changes before final orders are cut. While this can lead to significant angst, it is important to recognize that this occurs all across the Navy. Remember, Navy orders can always be changed until the moment of execution!
JUNIOR UMO TOUR:
The junior UMO tour is variable based upon the billet location and type. While the specifics of each job will vary, there are a few aspects that are constant.
Junior UMO tour orders are for 2.5-3 years.
This means that for those UMO students in the summer class, you are able to complete your entire UMO requirement in 2.5 years and return to residency at that point. The winter class is only able to complete 2 years of their requirement, and if they wish to return at 3 years, must apply for a waiver of their commitment. Otherwise, they will spend 3 years at their job with a year of training (4 years total). While it is encouraged by BUMED and the Detailer to extend for the purposes of maintaining manning, some residencies are more receptive to extensions than others.
The Job of a junior UMO is to do Special Duty Physicals, supervise IDCs, and run medical programs.
There is a wide range among UMO billets in the number of patients, sick call visits, and special duty physicals daily. Being proficient at special duty physicals is what Navy Medicine expects, and will be a significant part of your job as a junior UMO. Similarly, overseeing the IDC program takes up a large proportion of a UMO’s time because of the role IDCs play in patient care. You must train them to be as independent as possible, because they work under your license with little oversight on a submarine or during austere operations.
Decide how operational you wish to be.
In general, clinic, submarine, and education jobs do not deploy, while Navy Expeditionary Combat Command (NECC), NSW, and Marine Diving billets will deploy. If you wish to do so, however, there are opportunities to be more operational from any billet. The unique training section below covers some opportunities to be operational/underway, and can be a good way to supplement a more clinic-oriented position. Getting involved with the local dive locker can also be a way to supplement a clinic-based role.
SUBMARINE WARFARE QUALIFICATION:
The Submarine Warfare Qualification is the main Additional Qualification Designator (AQD), and the only warfare qualification available solely to UMOs. Completion of a three-part process is required to achieve the Submarine Medical Officer (SMO) qualification. This process is overseen by NUMI instruction 5420.2 (series). Each applicant must complete the SMO Qualification Examination with an 80% or better. It can be requested from the current NUMI Instructor (UMO) at any time during the tour. They must also complete 30 days underway, or 15 days for those at commands without submarine responsibilities. This underway time includes completion of a SMO qualification card, including a formal board while underway. This time can be challenging to complete for some billets, and waivers will be considered for specific reasons outlined in the instruction above.
Finally, a technical paper or thesis is required to complete the SMO qualification. This process can be more challenging and should be started as early as is possible. The topic must be related to submarine medicine, diving medicine, special operations medicine, or radiation health. Once a topic is devised, approval for the topic should be sought by submitting a brief proposal with a comprehensive bibliography. The ultimate thesis format and substance is explained within NUMIINST 5420.2, however it can be summarized as similar to a scientific paper in length, content, and requirements. Once all of these requirements are met, a final application for recognition of your warfare qualification completes the process.
RETURNING TO RESIDENCY:
There are two schools of thought during the UMO tour. One mindset to have is to read voraciously, seen patients, and maintained your skills in medicine as well as possible. Another method would be to enjoy yourself and the break from training, take care of the sailors at your command, and focus on being an exceptional Naval Officer.
If you want to stay current, there is limited funding from BUMED for physicians stationed at non-BSO-18 commands to attend conferences. There are also opportunities for permissive TAD for the purpose of educational opportunities that are advancing of your skills but not necessarily for your command. Moonlighting is also possible with specific permission from the CO and a state license (see MANMED and your local JAGyou’re your moonlighting instruction). Specialty specific resources are available, and you should seek out those from leaders/contacts in your chosen specialty. The UMO tour is a good time to shadow physicians in your specialty, attend academic conference (if feasible), and demonstrate sustained interest. Nearby MTFs can be useful places to stay involved, and there is often command support for maintaining relationships with local MTFs for the purpose of staying current.
UMOs tend to match well for competitive specialties as we tend to be motivated, self-starters with “fleet time” that is highly regarded on GME applications. If you are unsure of making the Navy a career, you can complete four years of HPSP obligation with one UMO tour and attempt to match in a civilian residency. You will have military experience and maturity when matching to civilian residencies; however, you will be somewhat older than your classmates and may need to repeat an internship (depending on which specialty you choose). Whether matching civilian or military, you have a lot going for your application, but without displaying interest in some fashion it can be challenging to match.
HYPERBARICS FELLOWSHIP:
If you desire further training in diving and hyperbaric medicine, you can apply for a fellowship in hyperbaric medicine. This gives you more exposure to the hyperbaric side of the specialty (the Navy training weighs more heavily on dive medicine), opens senior UMO billets up to you, and gives you an additional skill for transition to civilian life. The major locations for fellowship are University of California, San Diego, Duke University (Durham, NC), and Louisiana State University (New Orleans, LA). They typically last for one year and are a good opportunity to get paid a full-time Navy salary while “playing civilian.” If interested, seek out fellowship-trained UMOs for specific details. Of note, in order to qualify for a fellowship, you must be residency trained in a primary specialty. Typical primary specialties for hyperbaric fellowship are Emergency Medicine, Anesthesia, and Primary Care (IM/FP). In order to be competitive for selection by the Navy, you will need to have your Submarine Medical Warfare qualification as well as board certification in your primary specialty.
SENIOR UMO TOUR:
As with all operational medicine tours, there are opportunities to return to the community to serve in a senior UMO role. Group level billets exist for submarines and EOD as well as SMO billets at NSW commands. Some senior jobs require the hyperbaric fellowship (NDSTC, NAMI, NEDU), but most are open to any senior UMO. Most specialties will require a utilization tour in that specialty prior to embarking on a senior UMO tour. You must communicate your desire to leave your primary specialty with your Specialty Leader, be granted authorization to leave the specialty for a tour, and plan on returning to your primary specialty after your UMO tour. These jobs typically involve meetings, medical admin, setting policy for subordinate units, as well as medical oversight of junior medical officers and IDCs. If ultimately interested in this type of role, completing the Submarine Medical Officer Qualification while a junior-UMO is highly encouraged (if not required).
UNIQUE TRAINING OPPORTUNITIES:
- SAT DIVING/AQUARIUS: While the saturation diving program has not been functioning for some time, there has been an effort to revive the Saturation Fly-Away Diving System (SAT FADS), a mobile saturation diving unit built to sustain 6 divers to depths of 1,000fsw for 21 days with 9 subsequent days of decompression. Similarly, the US Navy has had a relationship with the Florida International University Aquarius program, an underwater habitat for saturation diving that has utility for human physiology studies as well as USN training. Introduction to these fields usually starts with a saturation diving course, which runs intermittently at NEDU; contact the UMO at NEDU for more information.
- Dry Deck Shelter (DDS): The US Navy supports Dry Deck Shelter (DDS) operations for launching and recovering of Navy Personnel, SEAL Delivery Vehicles, and Underwater Unmanned Vehicles from Submarines. Training in DDS operations happens intermittently, and can be coordinated with the UMOs at the Seal Delivery Vehicle Team 1 in Pearl Harbor, HI or via Naval Special Warfare Group 3.
- BIENNIAL ICEX: The US Navy does biennial ICE Exercises (ICEX) for evaluation of US Navy Submarine readiness in the unique environment of the Arctic. This is a multinational effort, which allows for multiple UMOs to be involved in either ICE Diving or submarine operations in the arctic. These are extremely unique opportunities only offered to UMOs, and more information can be found via the Arctic Submarine Laboratory (ASL) or the Underwater Warfighting Development Center (UWDC). These operations happen on even years.
- ICE DIVING: The cold water/ice diving course is a course designed to teach you the basics of setting up a dive side on the ice, diving in cold water environments – including the use of a dry suit – and managing the dive side in this environment. This course is offered by the Coast Guard and attended by Navy personnel.
Throwback Thursday Classic Post – The Book – Chapter 3 – Career Progression and Promotion Board Math
Introduction
When you start your Naval career, the future is largely a mystery. As you progress in your career, things will crystalize, you’ll become wiser, and you’ll think, “It would have been nice to know all of this in the beginning.”
I’m going to try and tell you what you should have known about career progression and promotion board math from the beginning.
Career Progression
This diagram below demonstrates the typical career progression of a Medical Corps officer who has no prior service. Assuming you are not picked early for promotion, you typically promote every six years. You will become a Lieutenant Commander (LCDR) at approximately 6 years, a Commander (CDR) at 12 years, and a Captain (CAPT) at 18 years. I had no prior service, I have never been promoted early, and this is exactly the timing I experienced in my career.
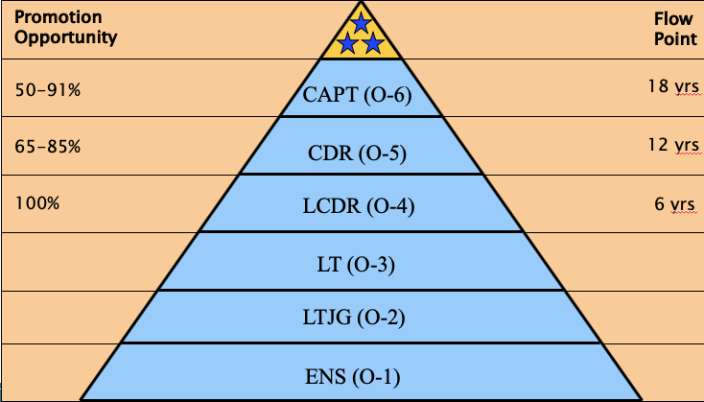
Along the left are the ranges of promotion opportunity for each rank from fiscal year 2010-2021. In each year, the promotion opportunity for LCDR has been 100%. In theory, if all the Lieutenants are suitable for promotion they can all be promoted to LCDR. When it comes to the promotion opportunities for CDR or CAPT, interpreting them is a touch more difficult because we have to talk about promotion board math.
Promotion Board Math
In Fiscal Year 2019 (FY19), people were very excited about a 90% promotion opportunity for the FY19 Staff Corps O6 promotion board. But it was easy to misinterpret this opportunity. It did not mean that 90% of CDRs were selected for CAPT.
Where Does the Promotion Opportunity Come From?
The short answer is from manpower projections. How many physicians are getting out or retiring? What is the current Medical Corps manning level for that rank? What are future needs anticipated to be? What is the size of the promotion zone? The answers to all of these questions determines the promotion opportunity and guide Navy Personnel Command (NPC) and the Bureau of Medicine and Surgery (BUMED) when they are making their decision.
As you can see here, the promotion opportunity varies from year-to-year:
| FY10 | FY11 | FY12 | FY13 | FY14 | FY15 | FY16 | FY17 | FY18 | FY19 | FY20 | FY21 | |
| LCDR | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | 100% | |
| CDR | 80% | 80% | 80% | 80% | 80% | 70% | 70% | 65% | 75% | 85% | 77% | |
| CAPT | 80% | 80% | 80% | 60% | 60% | 60% | 50% | 70% | 80% | 90% | 81% | 91% |
Historical promotion opportunities for FY10-21.
But as you can see here, the percentage who are promoted from the in zone group is substantially lower:
| FY10 | FY11 | FY12 | FY13 | FY14 | FY15 | FY16 | FY17 | FY18 | FY19 | FY20 | FY21 | |
| LCDR | N/A | N/A | N/A | 97% | 89% | 90% | 93% | 88% | 85% | 87% | 91% | |
| CDR | N/A | N/A | N/A | 58% | 66% | 49% | 53% | 44% | 40% | 52% | 53% | |
| CAPT | N/A | N/A | N/A | 55% | 43% | 47% | 39% | 34% | 37% | 41% | 51% | 53% |
Historical percentage of in-zone candidates selected for promotion for FY10-21.
Promotion Board Zones
There are three “zones” for promotion – below zone, in zone, and above zone. Medical Corps officers are below zone for two years, in zone for one year, and above zone until they are either selected for promotion or get out of the Navy. A few people are usually picked early or below zone, but most people will not get picked until they are in or above zone.
FY19 O6 Promotion Board Math
In FY19, there were 74 CDRs in zone for promotion. To figure out how many officers can be selected for promotion, you have to multiple the zone size by the promotion opportunity. For example, if you take the 90% promotion opportunity everyone was excited about and multiply it by the zone size of 74, you’ll see that they could have promoted 67 CDRs to CAPT during the board:
90% opportunity X 74 people in zone = 66.6 (rounded up to 67) people they can pick for O6
These 67, though, were picked from CDRs who were below zone, in zone, or above zone. Usually, there is a small number picked from below zone, and a much larger number from the in zone and above zone categories. Here were the results:
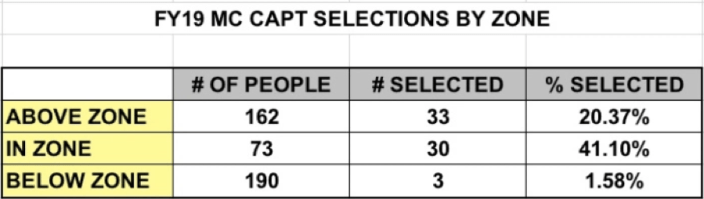
As you can see, the 90% promotion opportunity only led to a 41% selection rate for those who were in zone. The remainder came from the below and above zone CDRs.
The Bottom Line on Career Progression
The typical career progression occurs with a promotion every six years, as detailed in the diagram below. The promotion opportunities listed, though, result in a much lower chance of getting picked when you are in zone because the selections come from those below, in, and above zone.

Throwback Thursday Classic Post – MCCareer.org – The Book – Chapter 1 – What We Wish We Had Known
(Here’s a link to the “book”, which is really just my slow but steady attempt to organize all the content in an outline/book format.)
By Joel Schofer, MD, MBA, CPE, Paul Roszko, MD, Mickaila Johnston, MD, and Wendy Schofer, MD
As we look back at our Naval careers, these are things we wish we had known early in our career.
Medical School
- Going to the Uniformed Services University is great, but a seven year commitment is a long time unless you are 100% certain you want to do 20 years in the Navy (or will finish your time in the Reserves).
- If you want to improve your chances of matching in the internship/residency you want, you need to do everything you can to rotate there during your fourth year and impress them. Getting a publication or two before applying will also increase your competitiveness.
- If you ever fail a body composition assessment (BCA) or physical readiness test (PRT), your ability to promote to anything above LCDR will likely end for a five year period. For this reason, you need to make diet, exercise, and physical fitness part of your lifelong routine and NEVER fail a BCA or PRT.
- Make sure you save copies of your paperwork with the Navy, starting with the reimbursements/receipts during medical school and every Leave and Earning Statement (LES), which is the military pay stub. Sometimes errors are made and the only way to prove it is with your documentation.
- Do everything you can to live on the money you get when you’re in the Health Professions Scholarship Program (HPSP) and avoid taking out additional student loans. You want to make sure that you graduate medical school with as little additional loans as you can.
- Build wellness into your routine NOW. Take the stairs, make healthful food choices, drink water and don’t even start on diet sodas, build workouts into your schedule, and prioritize sleep. No one will do this for you. And PRTs are not workouts. You need to be active throughout the year, not just during PRT season.
Internship
- My Navy Portal is the centralized website that the Navy is developing as a one stop shop for all on-line websites you’ll need to access. In a similar manner, the My Navy Career Center is the one stop shop for any personnel questions you have. It can be reached at 833-330-MNCC or 901-874-MNCC (DSN 882-5672). You can also e-mail them at askmncc@navy.mil or live chat.
- If you want to be wealthy, you should save 20-30% of your gross (pre-tax) income for retirement. This is separate from any other savings for a house, cars, college, or anything else you are saving for. The 20-30% is exclusively for retirement. Add that to a military pension, and you’ll have options to retire early if you want to.
- Get a better understanding of finances and how the military retirement system works. Under the old retirement system, you received no contributions to your retirement unless you made them yourself. Familiarizing yourself with the Thrift Savings Plan (TSP) is even more important now with the Blended Retirement System (BRS) as the government now matches up to 5% of your base pay. This is free money, and everyone should know how to go into myPay and allocate a portion of their pay to their retirement account in the TSP.
- When investing in the TSP, it is easiest to only allocate a percentage of your base pay because it is more stable/predictable (i.e. you know how much is coming out of your paycheck and how much is going into your retirement account). Your special pays/bonuses will change more frequently, which can make it harder to ensure you are allocating enough money to maximize your yearly contributions.
- The Roth TSP is probably the better choice over the traditional TSP because your overall tax burden is relatively low, and certainly less than it would be if you were a full time physician outside of the military.
- If you do not know anything about investments, use of the Lifecycle funds is the easiest way to get started. They are the default option in the new BRS.
- If you are interested in research, most commands with graduate medical education (GME) programs will have a research office that holds sessions on how to get started conducting research. They can also help you secure external funding, however there are Surgeon General (SG) funds that are distributed through the Navy Medicine regions each year that you can apply for. Having an approved research proposal is usually the only barrier to getting access to these funds.
- Once you have completed your research project and wish to present your findings, you will need to obtain approval from your command before the manuscript, abstract, or poster is submitted to a conference or medical journal. You cannot publish anything in your official capacity without getting command approval and including the required disclaimers. Even presentations to the public need approval unless the audience is purely military.
- At some point during internship, you are going to want to download the Promo Prep, read it, and start updating your officer record, including getting an officer photo in your record. The sooner you can learn about this and get your record correct, the better. Some interns with prior service get considered for promotion to LCDR very early in their careers, so having a correct officer record that is ready for promotion boards should be a major goal of yours during the early phases of your Naval career.
- Create a CV and military bio and update them monthly for the rest of your career. You can find examples here. If you are interested in an academic career and promotion, you will need an educator’s portfolio as well. Since you will want to put all of your presentations in it and collect audience feedback/evaluations, the sooner you start doing this the more robust your portfolio will be when it is time for academic promotion.
- On a monthly basis, log on to SWANK, the Navy’s one-stop-shop for training requirements, and complete any training assigned to you.
- Learn the five critical fitness report mistakes and make sure none of them ever happen to you.
General Medical/Undersea Medical Officer and Flight Surgery Tours
- A non-medical reporting senior may not understand how to write your fitness report. The same can be said about inexperienced medical reporting seniors. You need to learn this yourself.
- Never let yourself get anything other than an Early Promote (EP) when you are getting a “one of one” fitrep.
- Always try to be above your reporting senior’s average.
- You may find yourself deploying for the first time. Make sure you read your orders. You may be able to break your lease and store your household goods and vehicle while you are gone. You should also consider investing up to $10,000 into the Savings Deposit Program (SDP), which provides a 10% guaranteed return on your money while you are deployed (and for 3 months after you return). This process cannot be initiated until you have had 30 days boots-on-ground and will need to be coordinated through the finance office where you are deployed. Also check to see if you qualify for the Combat Zone Tax Exemption (CZTE), which allows all of your earnings while deployed to be tax free. While entitled to the CZTE, any contributions to your Roth TSP are 100% tax free. If you can afford it, you can also contribute above the usual $19,000/year limit (in 2019). Once you have maximized your contributions to your Roth TSP, anything above $19,000 has to go into your traditional (non-Roth) TSP account.
Residency
- Travel for temporary additional duty (TAD) can very easily get screwed up. You are going to have to get familiar with the Defense Travel System (DTS) early on, so make sure you are really nice to the people in your travel office. They will have to teach you how the system works and what paperwork is required for you to travel.
- Be sure your Department Head and administrative assistants know your travel intentions well in advance so they can request the appropriate funds for their yearly budgets.
- Submit your DTS authorization request well in advance of your travel (> 90 days is preferable) because there will be mistakes or missing documentation you didn’t know you needed.
- Make sure you keep all relevant receipts from your travel (including SATO receipts for your airfare, hotel receipts, rental car receipts, registration for conferences, and parking receipts) and scan and upload them into DTS when you submit your voucher.
- If someone else wants to pay for you to travel, make sure to check with your legal office so you obtain the proper approvals.
- For all no-cost or permissive TAD travel, make sure a DTS request is entered and closed out after the travel. This is your way of documenting to the command where you went, for how long, and why you may have missed any command-wide required activities (e.g. urinalysis testing).
- Contact your Specialty Leader and Detailer 9-12 months ahead of your graduation date to start negotiating the orders for your utilization tour, but realize that most assignment decisions don’t get finalized until after the GME Selection Board results are finalized in January. Also realize that you are likely going to get what they give you when it comes to your first staff assignment. You may have some wiggle room to negotiate, but the most effective response to wherever they want to send you is most likely to be “Yes, Sir/Ma’am.” Bloom where you are planted.
- If you plan on making the Navy a career and having a family, it is probably easier to go overseas right out of residency, if possible. The more senior you get in the Navy, the harder it seems to be to go OCONUS. Kids get older and more tied to friends/schools. Go OCONUS right away and get it over with.
- Start your special pays request before you leave your GME site. You may be going somewhere without expertise in Medical Corps pay issues.
- The Navy will not pay for your state medical licenses, but it will pay for your board examinations and Maintenance of Certification. This process is easy to screw up, though, and this most commonly happens when you do not get advance approval to take the test or cross fiscal years. The instruction for board certification reimbursement can be found on the Useful Documents tab on MCCareer.org.
- If you want to do a fellowship, discuss this with your Specialty Leader probably two years before you intend to apply. They can give you information about the likelihood you can get training in that specialty and put you in touch with the Specialty Leader of that subspecialty (if there is one). You should follow any advice that you are given to make yourself competitive for the fellowship and apply for the fellowship even if you are told that there will not be any fellowship spots that year. Things change and sometimes you might be selected as an alternate and get the opportunity to apply for your fellowship if not all other fellowship positions wind up being filled.
Fellowship
- If you are in a full-time outservice (FTOS) fellowship, you will probably get non-observed (NOB) fitness reports. Although non-observed, you can still enter comments in block 41. Make sure you put all of your achievements and accomplishments in it.
- Because you will likely be receiving NOB fitness reports, you need to realize that they can have a dramatic effect on your ability to promote. Going into a promotion board with NOB fitreps puts you at a disadvantage, therefore, the best time to do a fellowship is after you are selected for promotion to your next rank. That said, you often have to take the fellowship whenever it is available. If you do so, just realize that it may delay your promotion by a few years.
- Make sure you figure out if it would be advantageous to take a retention bonus (RB) before you start your fellowship. This whole issue is explained in this blog post.
Utilization Tour
- Find the special pays coordinator at your command and track your special pays application to completion.
- Your first and only initial job is to pass your boards. After that…
- When your senior leadership asks you to do something, the answer should be “Yes, Sir/Ma’am.” If it isn’t, it’ll hurt your career.
- When they need volunteers for something, you should volunteer. If you don’t, it’ll hurt your career.
- If they need you to deploy, deploy without question or argument. If they need a volunteer, volunteer. If you don’t, it’ll hurt your career. Do you see a pattern here?
- If you trained in a civilian program and are new to the military, you should strive to take some military courses that can help you understand the core principles behind battlefield medicine and what is being taught to Corpsmen and medics. Familiarize yourself with the concept of the Joint Trauma System (JTS), Committee on Tactical Combat Casualty Care (TCCC), and the JTS Clinical Practice Guidelines. Taking the Basic Medical Department Officer Course (BMDOC) on-line or a TCCC course early in your career is a good idea.
- If you are notified you are deploying, there are a few things you should do. First, find out what type of deployment it is. If it is associated with your platform or you will deploying as an individual augmentee (IA, https://www.public.navy.mil/ia/Pages/index.aspx), then you’ll be staying at your current command. If you are deploying in a Global Support Assignment (GSA) then you will be receiving orders to PCS from your current command to a new one, likely Expeditionary Combat Readiness Center (ECRC) in Norfolk, Virginia. This will be your military command while deployed, and then you’ll get new orders to PCS somewhere else (which could be back to your original command) when you return.
- If you have an office phone with a DSN number, set it up to forward calls to your spouse/significant other’s mobile phone before you deploy. This allows you to call the DSN number from a landline at the location where you are deployed and get forwarded to your loved one’s phone.
- While you may think that there is no way that you are staying in for a long-term Navy career, don’t ever cross opportunities off the list. It may wind up being an alternative option that you can use in the civilian world or it will be a good stepping stone for your Navy career.
- Build in time for your family. Give the Navy your all while you are at work, but when you come home, be present with your family/friends/pets. The Navy needs strong officers, but it does not *love* you. Your family loves you and needs you.
Mid-Career (O4/O5)
- Get a mentor. Or two. Or three. Figure out who or what you want to be in five years, and seek out those people. Ask them for advice and mentorship.
- What do you want out of your Navy career? No matter how much you enjoy the Navy, the Navy will not love you back. You need to ensure that there is a balance between your inputs into the career and the yields. No one says you have to stay in past your obligations – the best approach may be to stay in as long as it is fun.
- Transitioning to the reserves is an option, but the grass is not always greener on the other side. If you are considering departing active duty for the drilling reserves, touch base with someone who is currently drilling (and not just a recruiter) to find out the realistic obligations and community needs.
- You need to get some major collateral duties. Until the system changes, it is usually your leadership duties in addition to your clinical duties that allows you to stand out when they are ranking people for fitness reports. If you’d like to see a list of appropriate collateral duties, here they are.
- You should try to get in the Advanced Medical Department Officer Course (AMDOC). There is a misconception that it helps you promote, which it really doesn’t. What it does is teach you all the things you need to know to be a developing and effective leader in the Navy.
- If you are in the reserves by this point, say yes to opportunities. You will stand out very quickly in your career progression by taking leadership courses and diverse annual trainings, as well as mobilizations that arise.
- Think about moves – when is a good time to volunteer to move to make it easier for your family. Some PCS/orders are not foreseen, but volunteering at particular times can give you a leg up in planning for family relocations at better times (e.g. at natural transition times in school, like between elementary and middle, or between middle and high).
Senior Career (O5/O6)
- The Navy should be fun. If you don’t like your job, change it. The Navy lets us change jobs more than most civilian settings would, and you don’t have to start over in a new organization.
- If you’re interested in being an Executive Officer (XO) or Commanding Officer (CO), you need at least one successful tour in a senior job. These usually include being a Director, Chief Medical Officer (CMO), or Medical Executive Committee (MEC) President at a military treatment facility or Officer-in-Charge of a clinic. You also need to get your Executive Medicine Additional Qualification Designator (AQD).
- You should try to complete Joint Professional Military Education I by the time your O6 promotion board occurs. It is among the more impactful and beneficial educational paths you can take in Navy Medicine.
- Unless you really enjoy them, you should seriously consider stopping any collateral duties, committees, etc. that no longer show up on your fitness report. If it isn’t important enough to show up on there, it isn’t important enough to do. There are only 168 hours in the week.
Throwback Thursday Classic Post – MCCareer.org – “The Book”
The Navy does an okay job helping physicians plan their careers, but in my opinion this preparation can be a lot better. This is why I created Joel Schofer’s Promo Prep and subsequently MCCareer.org. By the time you progress in your Naval career and learn everything you need to know, it is often too late. Therefore it is the responsibility of those who are senior and have already learned this information to teach it to the next generation of Naval physicians before it is too late.
The modern adult learner has more educational methods at his/her disposal than ever before. Whether you like social media, such as Twitter or Facebook, prefer to listen to podcasts in your car while you are driving, or like traditional methods of learning, such as reading articles, you can find one of these sources to learn about almost any topic you can imagine. Yet even though traditional books seem to have fallen out of favor during the rise of social media, there is still something reassuring about reading a book. Putting information in a book validates it and provides some degree of credibility. So, despite the fact that blogs have partially replaced books and the MCCareer.org blog has taken off, I think a book that discusses Navy Medical Corps career planning will still be well received and a valuable resource, which is why I’m creating one. I hope you enjoy it, benefit from it, and, frankly, help me create it. Here’s how I see this going down…
Take a look at the chapter list on this page. If there is something on it that you feel particularly qualified to write, let me know. Just in case I get a lot of interest, make sure to tell me what makes you qualified. Together we’ll use anything that is already on this site and we’ll turn it into a chapter, posting it on the site so others can read and use it.
If you think there is something we’re missing, let me know.
No one will make any money on this. It’ll just be a useful resource for anyone who wants to use it, and we’ll have it available on the blog. Maybe once it is all done we’ll create a real book in print or e-book, but for now I’m planning just putting it on the blog for free.
2020 State of the Blog, the Facebook Group, and The Book
At the beginning of every year I give a general update on how the blog is doing. Enjoy!
Profit
As during previous years, profit was negative $99. I make no money on this, and it costs me $99/year.
Blog Traffic
Here’s a graph of blog traffic since the blog was started in mid-2015:
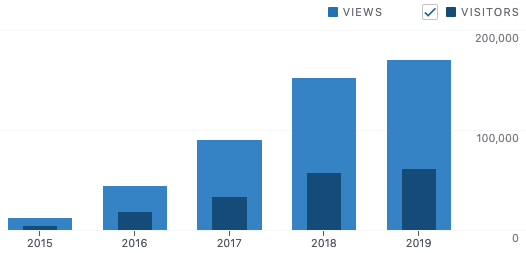
The lighter color is page views and the darker color is visitors:
- 2015 – 3,705 visitors viewed 10,870 pages with 66 posts published
- 2016 – 18,373 visitors viewed 43,673 pages with 133 posts published
- 2017 – 32,569 visitors viewed 88,263 pages with 194 posts published
- 2018 – 56,674 visitors viewed 151,044 pages with 212 posts published
- 2019 – 60,771 visitors viewed 169,684 pages with 371 posts published
10 Most Popular Blog Posts and Pages in 2019
Here are the 10 most popular pages and posts in 2019:
- Joel Schofer’s Promo Prep – 4,065 views
- LCDR Fitreps – Language for Writing Your Block 41 – 3,682 views
- Joel Schofer’s Fitrep Prep – 3,035 views
- Useful Documents – 2,791 views
- POM20 Navy Medicine Billet Reduction – 2,556 views
- CV, Military Bio, and Letter of Intent Templates – 2,367 views
- Useful Links – 1,989 views
- Personal Finance – 1,407 views
- What are AQDs and How Do You Get Them? – 1,223 views
- About Me – 1,083 views
MCCareer.org Private Facebook Group
Some of the blogs I read have vibrant forums and Facebook groups where members interact and ask each other questions. I once started a forum on MCCareer.org, but no one used it so I folded it up. I still have a private Facebook group, though, with over 260 members.
Despite people joining the Facebook group, no one ever posts comments or questions to it. I think there’s only been one in two years. Plenty of people contact me individually to ask questions, so I know there are a lot of questions out there. In 2020, I’d encourage readers to use the Facebook group to get opinions and answers from people other than me.
MCCareer.org “The Book”
Very slowly we’ve been posting “chapters” to the MCCareer.org “book.” Book is in quotes because it really isn’t a book, but more of a collection of on-line posts or chapters. Interest in writing “chapters” has been low so far, although a few authors other than me have pitched in. Most chapters thus far have been written by me.
I’ve begun the process of adding all of my posts to the book page, as you’ll see if you take a look. Slowly but surely I’ll fill out the content outline with what I’ve already written, and if there are holes I’ll write content to fill it in.
I considered creating a wiki page instead, but I’m not willing to give up editorial control. Occasionally someone will post something inappropriate to the blog, and I need to make sure nothing gets posted that would derail my Naval career.
Check out “The Book” when you get a chance and see if there is something you’d be interested in contributing. If there is, contact me.
MCCareer.org – The Book – Chapter 4 – Medical Corps Career Paths
By Joel Schofer, MD, MBA, CPE
(Note: The views expressed in this chapter are those of the author(s) and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.)
Introduction
There are many career paths available to Medical Corps officers. The five primary career paths include:
- Academic
- Administrative
- Clinical
- Operational
- Research
All of them can lead to promotion to O6. Here is a slide summarizing the Medical Corps career paths:

When comparing a Naval career to a civilian one, it is often easier to jump from one career path to another in the Navy than it would be in the civilian job market. All it takes is for you to take a new set of orders and you have switched career paths without having to start over. Let’s discuss the five career paths.
Academic Career Path
The academic career path involves much of the same activities as in the civilian world. You will largely be stationed at military treatment facilities (MTFs) with graduate medical education (GME) programs. In the Navy, these will include Family Medicine teaching hospitals/medical centers (Camp Lejeune, Camp Pendleton, Fort Belvoir, Jacksonville), Japanese MTFs with Japanese internships (Okinawa, Yokosuka), and medical centers with multiple residency programs and internships (Bethesda-Walter Reed, Portsmouth, San Diego). In addition, you could be stationed at the Uniformed Services University of the Health Sciences (USUHS) or in an educational support role at the Bureau of Medicine and Surgery (BUMED).
Aside from your clinical activity, you’ll be focusing on teaching and academic production. If you’re smart, you’ll work toward academic promotion in your department at USUHS by obtaining a faculty appointment (this newsletter tells you how to get one) and progressing toward academic promotion. Once you graduate from residency, you will likely be appointed an Assistant Professor, which means you are considered a local or regional expert. The next step would be to promote to Associate Professor, where you are a regional/national expert. Finally, you would strive for Professor, which usually indicates you are a national/international expert in your field.
If you receive a USUHS faculty appointment and, with the guidance of your USUHS department, actively work toward academic promotion, your academic career will be forced to progress. In my experience, most people obtain their initial appointment as an Assistant Professor but never progress from there. If you want to progress, you will need not only a curriculum vitae (CV) and biography, but also an educator’s portfolio. This portfolio can be a lot of work to create and maintain, and it is infinitely easier if you start early in your career.
The other relatively recent development in the academic career path is that there are many more options that are considered acceptable academic productivity. Traditionally, you had peer-reviewed publications and book chapters but little else. With the rise of the internet and social media, smartphone applications, blogs, podcasts, and other on-line options exist for you to produce academically and build your expertise and influence.
Research Career Path
The research career path is much like the academic one just discussed, but with a research focus. You would likely spend most of your career in MTFs with GME programs, but you can really do research anywhere in the Navy. Of particular interest, the Navy has commands whose primary missions are research, like Naval Health Research Center, Naval Medical Research Unit Dayton, and others.
Anyone planning a research career, you should strongly consider obtaining advance training. This could involve a fellowship, an advanced degree or certificate program, or additional continuing medical education. USUHS offers training in research.
Administrative Career Path
The administrative career path usually starts when you assume a leadership role appropriate for a junior to mid-grade officer. This would include Assistant Department Head, Department Head at a small/medium Military Treatment Facility (MTF), Medical Director, Senior Medical Officer, a leadership role on the Medical Executive Committee (MEC), or any other position where you assume administrative responsibility.
After the initial role, you gradually assume more responsibility, potentially at larger and at different types of commands. Although it is possible to obtain some of these roles as an O4, once you are selected to O5 a new world of positions is open to you that is easier to obtain as a CDR or CAPT. These would include Chair of a MEC committee, Department Head at a large MTF, Associate Director, Director, MEC Vice-President or President, Chief Medical Officer, Officer-in-Charge, or other positions with significant leadership roles. Once you are selected for O6, you can transition into Executive Medicine and can screen for Executive Officer and later Commanding Officer positions. If you are successful in your senior O6 leadership positions, you may be considered for promotion to the flag ranks as a Senior Healthcare Executive.
Many physicians who hope to rise to high levels of administration will try to increase their knowledge base by obtaining additional training. This can include military course like MedXellence or the Senior Officer Course in Military Justice and Civil Law. It can also include formal education in management and administration, such as a Master’s in Business Administration, Medical Management, or Healthcare Administration. There are many ways to obtain these degrees both inside and outside the service.
Clinical Career Path
The clinical career path is probably the purest and most natural career path. Why did you go to medical school? Usually, it is because you wanted to be a doctor, and the Navy needs people who want to be a doctor.
The first step in pursuing a career path is to complete a residency or fellowship in your desired field(s) of choice. After completing this graduate medical education, although not required by the Navy, you should strive to achieve board certification in these specialties, if available. First, it allows you to receive board certification pay. Second, it allows you to get a 5 in the professional expertise trait on your fitness report. Third, it is generally required to promote. Finally, when you moonlight or get out of the Navy, you will earn more than someone who is not board certified. And we all eventually get out of the Navy!
After achieving board certification, it is assumed that you will maintain it. In fact, it is required to continue receiving board certification pay. If you ever let your certification lapse, you must notify your special pays coordinator so they can terminate the board certification pay.
The downside of a purely clinical career path is that it can make it harder to promote to O6 if all you do is see patients and you are not willing to take on at least one significant collateral duty. I’m not saying it is impossible to promote as a pure clinician, but it can make it harder. On the positive side, a board certified clinician should be able to promote to O5, and some of the Commanders I know who are purely clinicians are some of the happiest physicians I know. You want me to join that committee? No thanks. I’m happy just being a doctor!
Operational Career Path
Many physicians pursue an operational career path because it is why they joined the military. You can be a doctor anywhere, but in the Navy you can be in submarines, dive, parachute, and all sorts of other fun and unique things.
An operational career path most commonly begins with a tour as a General Medical Officer (GMO) with the Marines or on a ship, a Flight Surgeon (FS), or Undersea Medical Officer (UMO). For those that go straight through in residency training, it may be that their first set of orders after residency takes them to an operational billet. In either case, physicians with an operational unit will probably find that they have a lot of responsibility for people with a work hard, play hard mentality. The 72 and 96 hour periods of leave that are common around holidays (play hard) are balanced by the requirement to deploy or train in the field (work hard).
As a physician promotes and becomes more senior, there are often opportunities to assume more senior roles specific to the operational community of choice. Along the way, it will be assumed that you are maintaining your clinical skills. Because it is often difficulty to maintain a full scope of practice in an operational setting, this may require extra effort to practice in a Military Treatment Facility or moonlight in your free time.
Summary
In summary, there are five primary career paths in the Navy. They include academic, administrative, clinical, operational, and research. In the Navy, it is usually fairly easy to transition from one career path to another without losing a step. Finally, pursuing all of them can lead to a fulfilling career and promotion to O6.
MCCareer.org The Book – Undersea Medicine Chapter
Brian M. Keuski, MD
Ian F. Eisenhauer, MD
Note: The views expressed in this chapter are those of the author(s) and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government.
INTRODUCTION TO UNDERSEA MEDICAL OFFICER (UMO):
Undersea Medicine is a small community within Navy Medicine, which primarily performs special duty physicals for divers, submariners, special operators, and nuclear-trained personnel. The Undersea Medical Officer (UMO) community, and those specialized communities that utilize UMOs, are high-tempo, actively deploying units ranging from Naval Special Warfare (NSW) to submarine squadrons. The role of the UMO is a mix of the general operational medicine that is expected of all General Medical Officers tailored to the specific duty concerns germane to the communities served. UMOs receive specialized training in these two key areas to ensure that they can adequately screen service members for conditions that could jeopardize the mission or lead to harm in diving, submarine or radiation health environments.
Medical administration (medical readiness, waivers/disqualifications, and the Independent Duty Corpsman (IDC) Program) takes up the majority of your time working as a UMO. UMOs train IDCs to tackle the challenging role of independent practice in austere environments with abbreviated training. UMOs must screen service members for illness that could overwhelm an IDC’s ability, as well as prepare IDCs to take care of those illnesses that arise with minimal access to MEDEVAC or specialty care. The key to success for a UMO will hinge directly on their ability to train those Dive Medical Technicians (DMTs) and IDCs who will ultimately perform patient care in the field.
UMO STRUCTURE AND JOB OPPORTUNITIES:
The UMO Community, as noted above, is a mix of submarine and diving support, organized by TYCOM-level leadership. UMOs fill billets assigned to the Marine Corps, Submarine Squadrons, Navy Special Warfare, Navy Expeditionary Combat Command (NECC), training commands, research commands, and Military Treatment Facilities as well as shipyard clinics. Most UMO roles are clinic-based. Completion of special duty physicals and leadership/mentorship of IDCs are the primary facets of the job. Some jobs incorporate diving into their role, while others have no associated diving. The many types of UMO billets are represented by categories, below.

The UMO Specialty Leader (M-95, Head Undersea Medicine) is located at the Bureau of Medicine and Surgery (BUMED) in Falls Church, Virginia, and oversees all of Radiation Health and Undersea Medicine. He/she makes recommendations to the waiver authority on all waivers and disqualifications of special duty standards. While all UMOs function under the oversight of the Specialty Leader, each has an operational chain of command. They either have a senior medical officer, or directly report as special staff to line officers in their daily duties. The above outline includes billets that are designated as senior officer billets, including some who are selected from the career milestone board, such as the Naval Undersea Medical Institute Officer-in-Charge (NUMI OIC) and Naval Submarine Medical Research Laboratory Commanding Officer and Executive Officer (NSMRL CO/XO), whereas others are open to any applicant. Second tour UMOs or senior UMOs will often have more opportunity to request billets, while those billets going to first tour UMOs will be chosen by the Detailer and Specialty Leader based upon their operational status, requirements, and “needs of the Navy.”
UMO APPLICATION:
UMO applications must be completed by the end of October, and selectees will be notified in December in parallel with graduate medical education (GME) selection. In order to prepare a successful application, UMO applicants must complete: a physical examination by a UMO (MANMED 15-102, 15-106), a passing Diver Candidate Physical Screening Test (PST) (MILPERSMAN 1220-410), two letters of recommendation, and a command letter of endorsement. A complete list of requirements can be found at the NUMI Website. Notably, these requirements represent minimum standards for training, but physical fitness well in excess of the minimums should be sought for a competitive application.
https://www.med.navy.mil/sites/nmotc/numi/UMOApply/Pages/default.aspx
Prospective UMOs historically have had the most difficulty with preparation for, and successful execution of the PST with a diver, as well as a letter of recommendation from qualified UMOs. The best resources for interns are nearby fleet UMOs or prior UMOs currently in GME training at your local MTF. These individuals can help you navigate the process, offer a recommendation letter, and administer your PST. If they can’t help you, the community is often small enough that they will know others that can. If no returning UMOs are within your intern class, ask upper level residents if they know any fleet returnees. Ultimately, the website above contains the contact information for the NUMI-POC, UMOC Mailbox, and the UMO Specialty Leader, each of whom will be willing to help you locate resources if you cannot otherwise. Letters of recommendation are also often difficult to complete. UMO letters of recommendation are designed to ensure you have considered why you are applying to the program, and to offer avenues for advice as you apply. If available during your intern program, scheduling an operational rotation with a local UMO can assist with the application requirements as well as show sustained interest.
The deadline for UMO application is in October; an interested applicant should complete the application in June-August to avoid an application being disqualified for missing requirements, including issues with medical standards that take time to process.
UMO PREPARATION:
Six months is a reasonable minimum amount of time to prepare for training prior to transferring to NUMI. Preparation must include learning multiple swim strokes, gaining in-water confidence, preparing to run significant distance, as well as improving callisthenic endurance. Below are outlined some minimum goals for reaching NUMI, though some factors that lead to success in school cannot be quantified. Ultimately, confidence in the water is the most important aspect of preparation for UMO training, and this takes time.
Be prepared to pass the PST with room to spare.
The Diver PST is a minimum standard that is used to ensure that candidates are ready to train. If you do not pass this ‘test’ on day one, you will be dismissed from training. Your swim will be in a cramped pool, with a shirt and UDTs on, and without goggles.
Some suggestions for success include:
- Train without goggles.
- Train in a crowded lane where you need to navigate around other swimmers.
- Swim with shorts and a baggy T-shirt to simulate the drag from the diver uniform.
- Become proficient, if not excellent, at sidestroke.
You also need to be prepared for the other events. Note that you will do your pull-ups after having just completed swimming, sit-ups, and push-ups. This fatigue causes issues for many people. Ten consecutive pull-ups prior to NUMI is a good minimum preparation for PST to compensate for this fatigue. If you currently can’t do any pull-ups, get multiple resistance bands, attach them to a pull-up bar (buy one and put it on your door – either at work or at home), and use as many bands as are necessary to be able to complete 6-8 pullups per set. When you can do 10 in a set, drop a band (or go to a smaller one). You should do pull-ups every other day, and you should do 50-60 at a minimum, which can be consecutive or broken up. If you do this for a few months, you will gain the required strength to do the pull-ups required for the PST.
Running is an important part of preparation for the PST. Being tired from upper body workouts and the aerobic stress of the pool will set you up to be slower than usual. You should be able to run your 1.5 miles in 11 minutes or under when you are fresh. Preparation can be with daily runs of 2-3 miles with 1 run per week designed to improve speed, and 1 run designed to improve distance. Examples of speed workouts may include Tabata runs or ¼ mile sprints, with a total distance of at least 1.5-2 miles (the length of the run portion of the PST) in sprints (e.g. 8 x ¼ mile sprints at goal pace, or under 1:50 per lap for an 11 minute time).
Be prepared to run for 5 miles at about an 8 minute mile pace.
While this may seem quick, you must recognize that you will be yelling cadences, running in formation, and carrying a guide-on flag. They will run you hard. Those who are unprepared for this type of distance often suffer stress injuries (shin splints, knee pain such as patellofemoral pain syndrome, etc.), so being prepared is crucial to making it through training. While at NUMI, they may not make you run this fast, but at NDSTC, some training teams will run significantly faster and farther.
Spend time doing hypoxia training (on land).
While breath-hold training in the water without supervision is dangerous, land-based training is very helpful in preparation for UMO training. There are many apps to teach you to hold your breath; STAmina Apnea Trainer, iHoldBreath, AIDA Freediving, and others. Having some comfort with a breath-hold allows a trainee to put their focus elsewhere during training. A 1:30 second breath-hold is a great starting place prior to starting at NUMI.
Get confident in the water.
You should be able to swim a minimum of 1000 meters in a workout, with mixed in push-ups, sit-ups, and pull-ups on the side of the pool. Calisthenic exercise mixed with swimming increases aerobic stress dramatically, and should be experienced before NUMI. Familiarity with breaststroke and freestyle are also useful, despite sidestroke and breaststroke being the only authorized swim strokes for the PST. Treading water is one of the most challenging factors of aquatic adaptability, and the eggbeater kick will make treading water easier. A trainee will need to be able to tread water with hands and elbows out of the water for a minimum of one minute. While methods other than eggbeater (frog kicks, flutter kicks, etc.) may seem easier at first, these methods break down when weight is held overhead. Becoming competent and confident while treading water will serve you well in training.
NUMI/NDSTC TRAINING PIPELINE, WHAT TO EXPECT:
The Naval Undersea Medicine Institute (NUMI) in Groton, CT is home to training for prospective Undersea Medical Officers. As noted above, preparation for this nearly six month training pipeline is crucial to success in becoming a UMO. The training pipeline is broken into three phases:
PHASE 1:
The First Phase of UMO Training is built around preparation for U.S. Navy Dive training at NDSTC. While there is a lot to learn to become an effective UMO, candidate failure is most often caused by quitting (drop on request -DOR) or an inability to meet the physical standards. Phase 1 physical preparation includes daily 1.5 hour workouts at 0500 to include running, calisthenics, swimming, in-water confidence training, practicing pool ‘hits,’ and other drills. The primary goals of UMOC preparation are PST preparation and in-water confidence training. This is where you will be introduced to over-unders, a repetitive under water swimming exercise. Preparation as noted above is highly encouraged to prepare you to start these exercises. While many UMOCs want to do over-unders prior to NUMI, the risk of shallow-water blackout is significant and has led to the death of skilled individuals. It is not recommended to do in water breath hold training before the safe training environment of NUMI. It is sufficient to become a great swimmer and have a good breath-hold prior to NUMI.
The time between workouts is spent learning radiation physics and health topics to complete the Radiation Health Indoctrination (RHI) certification. This certification prepares future UMOs to care for workers in the Radiation Health Program, as it allows UMOs to complete Radiation Medical Examinations (RMEs). This exam is required for Submarine personnel and Navy Divers who perform diving operations near submarines. The RHI Program also prepares UMOs to be the first line of defense in the event of a nuclear/radiologic casualty. Similarly, special duty physicals are introduced, an exam that certifies that specialized forces – including submariners, special warfare personnel, divers, radiation workers, and others – are able to complete their job effectively and safely without risking the safety of the mission or of the other crew.
UMOCs learn submarine medicine topics in phase I. In the submarine force, no person does a single job; it is the role of the entire crew to complete their main task, as well as to be prepared to address casualties, including fighting fires, addressing flooding, and even escaping the submarine. UMOCs complete training in these areas to understand ship systems and to be prepared to assist in these scenarios when/if they are aboard. UMOCs are also introduced to submarine culture and the hazards associated with submarine life.
PHASE 2:
The Second Phase of UMO training occurs on TAD orders to the Naval Diving and Salvage Training Center at the Center for Explosive Ordnance Disposal and Diving (CEODD). Prospective UMOs train like every other Navy Diver candidate with physical training both on land and in the water. Comfort in the water under extreme conditions is attained by breath-hold diving, treading with and without weights, surface swimming, teamwork drills, and many more activities. Training is built to ensure that candidates are sufficiently comfortable and calm in the water to train with equipment that can be dangerous if a diver were to panic. It should be noted that while traditionally this is where students fail out of the course, proper mental and physical preparation will prepare the vast majority of candidates.
The training includes qualification on the diving equipment used in the U.S. Navy. Competence with each piece of equipment is tested in both classroom and pool settings, to include SCUBA, KM-37 (Hard Hat Diving), and Mk-20 (full face-mask). There are also shorter familiarizations to re-breather equipment used by our forces. Most importantly for medical personnel, the course includes the Recognition and Treatment (R&T) of diving casualties course, which teaches candidates the medical knowledge required for treating diving related injuries. Topics span from basic dive physics to the latest theories on decompression sickness (aka ‘The Bends’), oxygen toxicity, and many other illnesses that can be seen in Navy Diving.
PHASE 3:
UMO training culminates in Groton, CT where comprehensive Oral Boards are performed for each candidate. Overseen by Naval Reactors, the nuclear power leadership of the U.S. Navy, this board includes questions about radiation health examinations, IDC oversight, special duty physicals, and diving related injuries. This phase also includes leadership education, operational medicine lectures, and helpful education in basic medical division officer roles and responsibilities. Most important to UMOs during this phase is assignment to a billet. While the process is variable, ranging from selection based upon course rank (merit-based) to direct assignment by the detailer, the process ultimately requires patience, as most UMOCs are post-intern physicians and have not yet experienced the flexible nature of Navy Orders. Once verbally assigned a billet, there are often multiple changes before final orders are cut. While this can lead to significant angst, it is important to recognize that this occurs all across the Navy. Remember, Navy orders can always be changed until the moment of execution!
JUNIOR UMO TOUR:
The junior UMO tour is variable based upon the billet location and type. While the specifics of each job will vary, there are a few aspects that are constant.
Junior UMO tour orders are for 2.5-3 years.
This means that for those UMO students in the summer class, you are able to complete your entire UMO requirement in 2.5 years and return to residency at that point. The winter class is only able to complete 2 years of their requirement, and if they wish to return at 3 years, must apply for a waiver of their commitment. Otherwise, they will spend 3 years at their job with a year of training (4 years total). While it is encouraged by BUMED and the Detailer to extend for the purposes of maintaining manning, some residencies are more receptive to extensions than others.
The Job of a junior UMO is to do Special Duty Physicals, supervise IDCs, and run medical programs.
There is a wide range among UMO billets in the number of patients, sick call visits, and special duty physicals daily. Being proficient at special duty physicals is what Navy Medicine expects, and will be a significant part of your job as a junior UMO. Similarly, overseeing the IDC program takes up a large proportion of a UMO’s time because of the role IDCs play in patient care. You must train them to be as independent as possible, because they work under your license with little oversight on a submarine or during austere operations.
Decide how operational you wish to be.
In general, clinic, submarine, and education jobs do not deploy, while Navy Expeditionary Combat Command (NECC), NSW, and Marine Diving billets will deploy. If you wish to do so, however, there are opportunities to be more operational from any billet. The unique training section below covers some opportunities to be operational/underway, and can be a good way to supplement a more clinic-oriented position. Getting involved with the local dive locker can also be a way to supplement a clinic-based role.
SUBMARINE WARFARE QUALIFICATION:
The Submarine Warfare Qualification is the main Additional Qualification Designator (AQD), and the only warfare qualification available solely to UMOs. Completion of a three-part process is required to achieve the Submarine Medical Officer (SMO) qualification. This process is overseen by NUMI instruction 5420.2 (series). Each applicant must complete the SMO Qualification Examination with an 80% or better. It can be requested from the current NUMI Instructor (UMO) at any time during the tour. They must also complete 30 days underway, or 15 days for those at commands without submarine responsibilities. This underway time includes completion of a SMO qualification card, including a formal board while underway. This time can be challenging to complete for some billets, and waivers will be considered for specific reasons outlined in the instruction above.
Finally, a technical paper or thesis is required to complete the SMO qualification. This process can be more challenging and should be started as early as is possible. The topic must be related to submarine medicine, diving medicine, special operations medicine, or radiation health. Once a topic is devised, approval for the topic should be sought by submitting a brief proposal with a comprehensive bibliography. The ultimate thesis format and substance is explained within NUMIINST 5420.2, however it can be summarized as similar to a scientific paper in length, content, and requirements. Once all of these requirements are met, a final application for recognition of your warfare qualification completes the process.
RETURNING TO RESIDENCY:
There are two schools of thought during the UMO tour. One mindset to have is to read voraciously, seen patients, and maintained your skills in medicine as well as possible. Another method would be to enjoy yourself and the break from training, take care of the sailors at your command, and focus on being an exceptional Naval Officer.
If you want to stay current, there is limited funding from BUMED for physicians stationed at non-BSO-18 commands to attend conferences. There are also opportunities for permissive TAD for the purpose of educational opportunities that are advancing of your skills but not necessarily for your command. Moonlighting is also possible with specific permission from the CO and a state license (see MANMED and your local JAGyou’re your moonlighting instruction). Specialty specific resources are available, and you should seek out those from leaders/contacts in your chosen specialty. The UMO tour is a good time to shadow physicians in your specialty, attend academic conference (if feasible), and demonstrate sustained interest. Nearby MTFs can be useful places to stay involved, and there is often command support for maintaining relationships with local MTFs for the purpose of staying current.
UMOs tend to match well for competitive specialties as we tend to be motivated, self-starters with “fleet time” that is highly regarded on GME applications. If you are unsure of making the Navy a career, you can complete four years of HPSP obligation with one UMO tour and attempt to match in a civilian residency. You will have military experience and maturity when matching to civilian residencies; however, you will be somewhat older than your classmates and may need to repeat an internship (depending on which specialty you choose). Whether matching civilian or military, you have a lot going for your application, but without displaying interest in some fashion it can be challenging to match.
HYPERBARICS FELLOWSHIP:
If you desire further training in diving and hyperbaric medicine, you can apply for a fellowship in hyperbaric medicine. This gives you more exposure to the hyperbaric side of the specialty (the Navy training weighs more heavily on dive medicine), opens senior UMO billets up to you, and gives you an additional skill for transition to civilian life. The major locations for fellowship are University of California, San Diego, Duke University (Durham, NC), and Louisiana State University (New Orleans, LA). They typically last for one year and are a good opportunity to get paid a full-time Navy salary while “playing civilian.” If interested, seek out fellowship-trained UMOs for specific details. Of note, in order to qualify for a fellowship, you must be residency trained in a primary specialty. Typical primary specialties for hyperbaric fellowship are Emergency Medicine, Anesthesia, and Primary Care (IM/FP). In order to be competitive for selection by the Navy, you will need to have your Submarine Medical Warfare qualification as well as board certification in your primary specialty.
SENIOR UMO TOUR:
As with all operational medicine tours, there are opportunities to return to the community to serve in a senior UMO role. Group level billets exist for submarines and EOD as well as SMO billets at NSW commands. Some senior jobs require the hyperbaric fellowship (NDSTC, NAMI, NEDU), but most are open to any senior UMO. Most specialties will require a utilization tour in that specialty prior to embarking on a senior UMO tour. You must communicate your desire to leave your primary specialty with your Specialty Leader, be granted authorization to leave the specialty for a tour, and plan on returning to your primary specialty after your UMO tour. These jobs typically involve meetings, medical admin, setting policy for subordinate units, as well as medical oversight of junior medical officers and IDCs. If ultimately interested in this type of role, completing the Submarine Medical Officer Qualification while a junior-UMO is highly encouraged (if not required).
UNIQUE TRAINING OPPORTUNITIES:
- SAT DIVING/AQUARIUS: While the saturation diving program has not been functioning for some time, there has been an effort to revive the Saturation Fly-Away Diving System (SAT FADS), a mobile saturation diving unit built to sustain 6 divers to depths of 1,000fsw for 21 days with 9 subsequent days of decompression. Similarly, the US Navy has had a relationship with the Florida International University Aquarius program, an underwater habitat for saturation diving that has utility for human physiology studies as well as USN training. Introduction to these fields usually starts with a saturation diving course, which runs intermittently at NEDU; contact the UMO at NEDU for more information.
- Dry Deck Shelter (DDS): The US Navy supports Dry Deck Shelter (DDS) operations for launching and recovering of Navy Personnel, SEAL Delivery Vehicles, and Underwater Unmanned Vehicles from Submarines. Training in DDS operations happens intermittently, and can be coordinated with the UMOs at the Seal Delivery Vehicle Team 1 in Pearl Harbor, HI or via Naval Special Warfare Group 3.
- BIENNIAL ICEX: The US Navy does biennial ICE Exercises (ICEX) for evaluation of US Navy Submarine readiness in the unique environment of the Arctic. This is a multinational effort, which allows for multiple UMOs to be involved in either ICE Diving or submarine operations in the arctic. These are extremely unique opportunities only offered to UMOs, and more information can be found via the Arctic Submarine Laboratory (ASL) or the Underwater Warfighting Development Center (UWDC). These operations happen on even years.
- ICE DIVING: The cold water/ice diving course is a course designed to teach you the basics of setting up a dive side on the ice, diving in cold water environments – including the use of a dry suit – and managing the dive side in this environment. This course is offered by the Coast Guard and attended by Navy personnel.
MCCareer.org The Book – Chapter 3 – Career Progression and Promotion Board Math
Introduction
When you start your Naval career, the future is largely a mystery. As you progress is your career, things will crystalize, you’ll become wiser, and you’ll think, “It would have been nice to know all of this in the beginning.”
I’m going to try and tell you what you should have known about career progression and promotion board math from the beginning.
Career Progression
This diagram below demonstrates the typical career progression of a Medical Corps officer who has no prior service. Assuming you are not picked early for promotion, you typically promote every six years. You will become a Lieutenant Commander (LCDR) at approximately 6 years, a Commander (CDR) at 12 years, and a Captain (CAPT) at 18 years. I had no prior service, I have never been promoted early, and this is exactly the timing I experienced in my career.

Along the left are the ranges of promotion opportunity for each rank from fiscal year 2013-2020. In each year, the promotion opportunity for LCDR has been 100%. In theory, if all the Lieutenants are suitable for promotion they can all be promoted to LCDR. When it comes to the promotion opportunities for CDR or CAPT, interpreting them is a touch more difficult because we have to talk about promotion board math.
Promotion Board Math
In Fiscal Year 2019 (FY19), people were very excited about a 90% promotion opportunity for the FY19 Staff Corps O6 promotion board. But it was easy to misinterpret this opportunity. It did not mean that 90% of CDRs were selected for CAPT.
Where Does the Promotion Opportunity Come From?
The short answer is from manpower projections. How many physicians are getting out or retiring? What is the current Medical Corps manning level for that rank? What are future needs anticipated to be? What is the size of the promotion zone? The answers to all of these questions determines the promotion opportunity and guide Navy Personnel Command (NPC) and the Bureau of Medicine and Surgery (BUMED) when they are making their decision.
As you can see here, the promotion opportunity varies from year-to-year:
| FY13 | FY14 | FY15 | FY16 | FY17 | FY18 | FY19 | FY20 | |
| LCDR | 100% | 100% | 100% | 100% | 100% | 100% | 100% | Pending |
| CDR | 80% | 80% | 70% | 70% | 65% | 75% | 85% | 77% |
| CAPT | 60% | 60% | 60% | 50% | 70% | 80% | 90% | 81% |
Historical promotion opportunities for FY13-20.
But as you can see here, the percentage who are promoted from the in zone group is substantially lower:
| FY13 | FY14 | FY15 | FY16 | FY17 | FY18 | FY19 | FY20 | |
| LCDR | 97% | 89% | 90% | 93% | 88% | 85% | 87% | Pending |
| CDR | 58% | 66% | 49% | 53% | 44% | 40% | 52% | 53% |
| CAPT | 55% | 43% | 47% | 39% | 34% | 37% | 41% | 51% |
Historical percentage of in-zone candidates selected for promotion for FY13-20.
Promotion Board Zones
There are three “zones” for promotion – below zone, in zone, and above zone. Medical Corps officers are below zone for two years, in zone for one year, and above zone until they are either selected for promotion or get out of the Navy. A few people are usually picked early or below zone, but most people will not get picked until they are in or above zone.
FY19 O6 Promotion Board Math
In FY19, there were 74 CDRs in zone for promotion. To figure out how many officers can be selected for promotion, you have to multiple the zone size by the promotion opportunity. For example, if you take the 90% promotion opportunity everyone was excited about and multiply it by the zone size of 74, you’ll see that they could have promoted 67 CDRs to CAPT during the board:
90% opportunity X 74 people in zone = 66.6 (rounded up to 67) people they can pick for O6
These 67, though, were picked from CDRs who were below zone, in zone, or above zone. Usually, there is a small number picked from below zone, and a much larger number from the in zone and above zone categories. Here were the results:

As you can see, the 90% promotion opportunity only led to a 41% selection rate for those who were in zone. The remainder came from the below and above zone CDRs.
The Bottom Line on Career Progression
The typical career progression occurs with a promotion every six years, as detailed in the diagram below. The promotion opportunities listed, though, result in a much lower chance of getting picked when you are in zone because the selections come from those below, in, and above zone.

MCCareer.org – The Book – Chapter 1 – What We Wish We Had Known
By Joel Schofer, MD, MBA, CPE, Paul Roszko, MD, Mickaila Johnston, MD, and Wendy Schofer, MD
As we look back at our Naval careers, these are things we wish we had known early in our career.
Medical School
- Going to the Uniformed Services University is great, but a seven year commitment is a long time unless you are 100% certain you want to do 20 years in the Navy (or will finish your time in the Reserves).
- If you want to improve your chances of matching in the internship/residency you want, you need to do everything you can to rotate there during your fourth year and impress them. Getting a publication or two before applying will also increase your competitiveness.
- If you ever fail a body composition assessment (BCA) or physical readiness test (PRT), your ability to promote to anything above LCDR will likely end for a five year period. For this reason, you need to make diet, exercise, and physical fitness part of your lifelong routine and NEVER fail a BCA or PRT.
- Make sure you save copies of your paperwork with the Navy, starting with the reimbursements/receipts during medical school and every Leave and Earning Statement (LES), which is the military pay stub. Sometimes errors are made and the only way to prove it is with your documentation.
- Do everything you can to live on the money you get when you’re in the Health Professions Scholarship Program (HPSP) and avoid taking out additional student loans. You want to make sure that you graduate medical school with as little additional loans as you can.
- Build wellness into your routine NOW. Take the stairs, make healthful food choices, drink water and don’t even start on diet sodas, build workouts into your schedule, and prioritize sleep. No one will do this for you. And PRTs are not workouts. You need to be active throughout the year, not just during PRT season.
Internship
- My Navy Portal is the centralized website that the Navy is developing as a one stop shop for all on-line websites you’ll need to access. In a similar manner, the My Navy Career Center is the one stop shop for any personnel questions you have. It can be reached at 833-330-MNCC or 901-874-MNCC (DSN 882-5672). You can also e-mail them at askmncc@navy.mil or live chat.
- If you want to be wealthy, you should save 20-30% of your gross (pre-tax) income for retirement. This is separate from any other savings for a house, cars, college, or anything else you are saving for. The 20-30% is exclusively for retirement. Add that to a military pension, and you’ll have options to retire early if you want to.
- Get a better understanding of finances and how the military retirement system works. Under the old retirement system, you received no contributions to your retirement unless you made them yourself. Familiarizing yourself with the Thrift Savings Plan (TSP) is even more important now with the Blended Retirement System (BRS) as the government now matches up to 5% of your base pay. This is free money, and everyone should know how to go into myPay and allocate a portion of their pay to their retirement account in the TSP.
- When investing in the TSP, it is easiest to only allocate a percentage of your base pay because it is more stable/predictable (i.e. you know how much is coming out of your paycheck and how much is going into your retirement account). Your special pays/bonuses will change more frequently, which can make it harder to ensure you are allocating enough money to maximize your yearly contributions.
- The Roth TSP is probably the better choice over the traditional TSP because your overall tax burden is relatively low, and certainly less than it would be if you were a full time physician outside of the military.
- If you do not know anything about investments, use of the Lifecycle funds is the easiest way to get started. They are the default option in the new BRS.
- If you are interested in research, most commands with graduate medical education (GME) programs will have a research office that holds sessions on how to get started conducting research. They can also help you secure external funding, however there are Surgeon General (SG) funds that are distributed through the Navy Medicine regions each year that you can apply for. Having an approved research proposal is usually the only barrier to getting access to these funds.
- Once you have completed your research project and wish to present your findings, you will need to obtain approval from your command before the manuscript, abstract, or poster is submitted to a conference or medical journal. You cannot publish anything in your official capacity without getting command approval and including the required disclaimers. Even presentations to the public need approval unless the audience is purely military.
- At some point during internship, you are going to want to download the Promo Prep, read it, and start updating your officer record, including getting an officer photo in your record. The sooner you can learn about this and get your record correct, the better. Some interns with prior service get considered for promotion to LCDR very early in their careers, so having a correct officer record that is ready for promotion boards should be a major goal of yours during the early phases of your Naval career.
- Create a CV and military bio and update them monthly for the rest of your career. You can find examples here. If you are interested in an academic career and promotion, you will need an educator’s portfolio as well. Since you will want to put all of your presentations in it and collect audience feedback/evaluations, the sooner you start doing this the more robust your portfolio will be when it is time for academic promotion.
- On a monthly basis, log on to SWANK, the Navy’s one-stop-shop for training requirements, and complete any training assigned to you.
- Learn the five critical fitness report mistakes and make sure none of them ever happen to you.
General Medical/Undersea Medical Officer and Flight Surgery Tours
- A non-medical reporting senior may not understand how to write your fitness report. The same can be said about inexperienced medical reporting seniors. You need to learn this yourself.
- Never let yourself get anything other than an Early Promote (EP) when you are getting a “one of one” fitrep.
- Always try to be above your reporting senior’s average.
- You may find yourself deploying for the first time. Make sure you read your orders. You may be able to break your lease and store your household goods and vehicle while you are gone. You should also consider investing up to $10,000 into the Savings Deposit Program (SDP), which provides a 10% guaranteed return on your money while you are deployed (and for 3 months after you return). This process cannot be initiated until you have had 30 days boots-on-ground and will need to be coordinated through the finance office where you are deployed. Also check to see if you qualify for the Combat Zone Tax Exemption (CZTE), which allows all of your earnings while deployed to be tax free. While entitled to the CZTE, any contributions to your Roth TSP are 100% tax free. If you can afford it, you can also contribute above the usual $19,000/year limit (in 2019). Once you have maximized your contributions to your Roth TSP, anything above $19,000 has to go into your traditional (non-Roth) TSP account.
Residency
- Travel for temporary additional duty (TAD) can very easily get screwed up. You are going to have to get familiar with the Defense Travel System (DTS) early on, so make sure you are really nice to the people in your travel office. They will have to teach you how the system works and what paperwork is required for you to travel.
- Be sure your Department Head and administrative assistants know your travel intentions well in advance so they can request the appropriate funds for their yearly budgets.
- Submit your DTS authorization request well in advance of your travel (> 90 days is preferable) because there will be mistakes or missing documentation you didn’t know you needed.
- Make sure you keep all relevant receipts from your travel (including SATO receipts for your airfare, hotel receipts, rental car receipts, registration for conferences, and parking receipts) and scan and upload them into DTS when you submit your voucher.
- If someone else wants to pay for you to travel, make sure to check with your legal office so you obtain the proper approvals.
- For all no-cost or permissive TAD travel, make sure a DTS request is entered and closed out after the travel. This is your way of documenting to the command where you went, for how long, and why you may have missed any command-wide required activities (e.g. urinalysis testing).
- Contact your Specialty Leader and Detailer 9-12 months ahead of your graduation date to start negotiating the orders for your utilization tour, but realize that most assignment decisions don’t get finalized until after the GME Selection Board results are finalized in January. Also realize that you are likely going to get what they give you when it comes to your first staff assignment. You may have some wiggle room to negotiate, but the most effective response to wherever they want to send you is most likely to be “Yes, Sir/Ma’am.” Bloom where you are planted.
- If you plan on making the Navy a career and having a family, it is probably easier to go overseas right out of residency, if possible. The more senior you get in the Navy, the harder it seems to be to go OCONUS. Kids get older and more tied to friends/schools. Go OCONUS right away and get it over with.
- Start your special pays request before you leave your GME site. You may be going somewhere without expertise in Medical Corps pay issues.
- The Navy will not pay for your state medical licenses, but it will pay for your board examinations and Maintenance of Certification. This process is easy to screw up, though, and this most commonly happens when you do not get advance approval to take the test or cross fiscal years. The instruction for board certification reimbursement can be found on the Useful Documents tab on MCCareer.org.
- If you want to do a fellowship, discuss this with your Specialty Leader probably two years before you intend to apply. They can give you information about the likelihood you can get training in that specialty and put you in touch with the Specialty Leader of that subspecialty (if there is one). You should follow any advice that you are given to make yourself competitive for the fellowship and apply for the fellowship even if you are told that there will not be any fellowship spots that year. Things change and sometimes you might be selected as an alternate and get the opportunity to apply for your fellowship if not all other fellowship positions wind up being filled.
Fellowship
- If you are in a full-time outservice (FTOS) fellowship, you will probably get non-observed (NOB) fitness reports. Although non-observed, you can still enter comments in block 41. Make sure you put all of your achievements and accomplishments in it.
- Because you will likely be receiving NOB fitness reports, you need to realize that they can have a dramatic effect on your ability to promote. Going into a promotion board with NOB fitreps puts you at a disadvantage, therefore, the best time to do a fellowship is after you are selected for promotion to your next rank. That said, you often have to take the fellowship whenever it is available. If you do so, just realize that it may delay your promotion by a few years.
- Make sure you figure out if it would be advantageous to take a retention bonus (RB) before you start your fellowship. This whole issue is explained in this blog post.
Utilization Tour
- Find the special pays coordinator at your command and track your special pays application to completion.
- Your first and only initial job is to pass your boards. After that…
- When your senior leadership asks you to do something, the answer should be “Yes, Sir/Ma’am.” If it isn’t, it’ll hurt your career.
- When they need volunteers for something, you should volunteer. If you don’t, it’ll hurt your career.
- If they need you to deploy, deploy without question or argument. If they need a volunteer, volunteer. If you don’t, it’ll hurt your career. Do you see a pattern here?
- If you trained in a civilian program and are new to the military, you should strive to take some military courses that can help you understand the core principles behind battlefield medicine and what is being taught to Corpsmen and medics. Familiarize yourself with the concept of the Joint Trauma System (JTS), Committee on Tactical Combat Casualty Care (TCCC), and the JTS Clinical Practice Guidelines. Taking the Basic Medical Department Officer Course (BMDOC) on-line or a TCCC course early in your career is a good idea.
- If you are notified you are deploying, there are a few things you should do. First, find out what type of deployment it is. If it is associated with your platform or you will deploying as an individual augmentee (IA, https://www.public.navy.mil/ia/Pages/index.aspx), then you’ll be staying at your current command. If you are deploying in a Global Support Assignment (GSA) then you will be receiving orders to PCS from your current command to a new one, likely Expeditionary Combat Readiness Center (ECRC) in Norfolk, Virginia. This will be your military command while deployed, and then you’ll get new orders to PCS somewhere else (which could be back to your original command) when you return.
- If you have an office phone with a DSN number, set it up to forward calls to your spouse/significant other’s mobile phone before you deploy. This allows you to call the DSN number from a landline at the location where you are deployed and get forwarded to your loved one’s phone.
- While you may think that there is no way that you are staying in for a long-term Navy career, don’t ever cross opportunities off the list. It may wind up being an alternative option that you can use in the civilian world or it will be a good stepping stone for your Navy career.
- Build in time for your family. Give the Navy your all while you are at work, but when you come home, be present with your family/friends/pets. The Navy needs strong officers, but it does not *love* you. Your family loves you and needs you.
Mid-Career (O4/O5)
- Get a mentor. Or two. Or three. Figure out who or what you want to be in five years, and seek out those people. Ask them for advice and mentorship.
- What do you want out of your Navy career? No matter how much you enjoy the Navy, the Navy will not love you back. You need to ensure that there is a balance between your inputs into the career and the yields. No one says you have to stay in past your obligations – the best approach may be to stay in as long as it is fun.
- Transitioning to the reserves is an option, but the grass is not always greener on the other side. If you are considering departing active duty for the drilling reserves, touch base with someone who is currently drilling (and not just a recruiter) to find out the realistic obligations and community needs.
- You need to get some major collateral duties. Until the system changes, it is usually your leadership duties in addition to your clinical duties that allows you to stand out when they are ranking people for fitness reports. If you’d like to see a list of appropriate collateral duties, here they are.
- You should try to get in the Advanced Medical Department Officer Course (AMDOC). There is a misconception that it helps you promote, which it really doesn’t. What it does is teach you all the things you need to know to be a developing and effective leader in the Navy.
- If you are in the reserves by this point, say yes to opportunities. You will stand out very quickly in your career progression by taking leadership courses and diverse annual trainings, as well as mobilizations that arise.
- Think about moves – when is a good time to volunteer to move to make it easier for your family. Some PCS/orders are not foreseen, but volunteering at particular times can give you a leg up in planning for family relocations at better times (e.g. at natural transition times in school, like between elementary and middle, or between middle and high).
Senior Career (O5/O6)
- The Navy should be fun. If you don’t like your job, change it. The Navy lets us change jobs more than most civilian settings would, and you don’t have to start over in a new organization.
- If you’re interested in being an Executive Officer (XO) or Commanding Officer (CO), you need at least one successful tour in a senior job. These usually include being a Director, Chief Medical Officer (CMO), or Medical Executive Committee (MEC) President at a military treatment facility or Officer-in-Charge of a clinic. You also need to get your Executive Medicine Additional Qualification Designator (AQD).
- You should try to complete Joint Professional Military Education I by the time your O6 promotion board occurs. It is among the more impactful and beneficial educational paths you can take in Navy Medicine.
- Unless you really enjoy them, you should seriously consider stopping any collateral duties, committees, etc. that no longer show up on your fitness report. If it isn’t important enough to show up on there, it isn’t important enough to do. There are only 168 hours in the week.
Tell Me What You Wish You Had Known
The first chapter of the planned MCCareer.org book is “I Wish I Had Known”. Let’s write it!
Reflect on your career and tell me what you wish you had known when you were younger, more junior in rank, and (in my case) had more hair. You can tell me using the contact me tab, Tweet me, Facebook me, contact me on LinkedIn, or post it in the comments below this post. If I like your suggestions, you’ll get credited in the chapter. In fact, if you contribute enough you might become a co-author!